Hydrocephalus Monitoring Reports & Findings with the DiaCeph Test
 Permission granted to publish
these reports.
Permission granted to publish
these reports.
If you prefer, you may view/download our Two Hydrocephalus Monitoring Reports on SlideShare.net
Hydrocephalus Monitoring Reports & Results
This monitoring is based on my DiaCeph monitoring system, and many years and experience in hydrocephalus care and research. In my 17 years of nuclear medicine imaging work, 10 of those years where I owned my own company, Certified Nuclear Imaging, I worked up approximately 15, 000 patients for a variety of illnesses including cancer, heart disease, and hydrocephalus. I regularly authored procedures in this space, and have provided services to more than 50 facilities. I am also a "medical intuitive." In my nuclear medicine imaging work from 1981 to 1992, I routinely applied "intuitive reads" to my medical work-ups, and my intuitive reads matched the actual clinical test results about 80% of the time. I bring this up as I am comfortable including intuitive reads where applicable, and upon request. In May 2010, I conducted a group drumming event for the UCI Susan Samueli Integrative Medicine Center, and this center has been inquiring as to "intuitive" services I might be available to do. As a scientist, I will state that intuitive work has its place in medicine and wellness. Period.
In my neurological and neuroscience efforts since my 1992 onset of hydrocephalus, I have conducted considerable shunt and neuroscience research in cognition and assistive technology, authored related papers, a 1996 FDA petition, guidance papers to FDA, and led and advised in civil proceedings of products liability and insurance bad faith issues. I have counseled others in legal proceedings both pro bono, and as a legal advocate and consultant.
Since 1976, I have rather extensive technical writing in support of medical products, medical applications, and medical procedures. As a result, I am also skilled in human factors engineering and product labeling - an area of great need today.
Typically, shunt monitoring would involve a 3rd party to provide user instruction to a patient or family. Someone would need to instruct/train the physician on how to interpret the results. The insurance company would need to pay the physician to process and interpret the results. The insurance company would also need to pay for the device rental and testing, often an area where 3rd party contractors, consultants, and trainers are involved.
In my hydrocephalus monitoring consultations, I set up monitoring to address your specific hydrocephalus and shunt needs. I instruct you/your family how to do the monitoring, typically over 10 to 14 days. When the monitoring is complete, you return the materials to me, and I plug the data into my computer and generate graphs of your data. Then I prepare a report for you and your neurosurgeon. Unfortunately, this is not covered by insurance.
My consultations take between 5 and 10 hours. My fees are billed at $125.00/hour, making the total cost between $625.00 and $1250.00, but often I can do it in 5 hours. I can also speak to your doctors. If you are interested in this monitoring, complete this Authorization to Release Health Records (PDF file) and Professional Services Agreement (PDF file), and mail them along with a check for $625.00 (5-hours of my time) to 3908 1/2 River Ave., Newport Beach, CA 92663. If there are no additional complicating issues, in most cases I can complete the monitoring and report in the 5-hour period. Thank you. Stephen
DiaCeph Monitoring Consult Report (patient from Johns Hopkins Medical Center)
Reason for Consult:
The patient was diagnosed with NPH in February of 2009, and has undergone several surgical procedures to arrest his NPH related complaints. His NPH is complicated by blindness (retinitis pigmentosa) and prostate enlargement. Unsatisfied with his NPH outcome, he contacted me for a patient consult and to undertake non-invasive “DiaCeph” monitoring.
Materials:
1. Customized DiaCeph Monitoring Instructions for this NPH Patient, Color-Coded for Visual Impairment
2. Custom DiaCeph Monitoring Forms for this NPH Patient, Color-Coded for Visual Impairment
3. Assortment of hand percussion instruments - as part of my neuropsych and Integrative Medicine evaluation
NPH Illness, Surgical History, and Discussion:
The patient was tentatively diagnosed with normal pressure hydrocephalus in Dec. 2008 on an MRI brain scan. He was evaluated clinically by his Internist on 2/25/09, and admitted to the Johns Hopkins neurology unit on 3/13/09 for a CSF drainage trial by his neurologist, where withdrawal of 547 cc of CSF produced a positive response. It was felt, based on that evaluation that the patient’s gait and walking would benefit from CSF diversion surgery, but that his urinary urgency and mild cognitive complaints would likely be unaffected. CT and MRI brain scans demonstrated mild to moderate ventriculomegaly consistent with NPH, and ischemic vessel changes thought related to age. His neurologist felt there was some mild cognitive impairment, more related to dementia than NPH. *An asterisk is added to his CSF drainage results as his report states that the patient’s baseline data was not obtained until after an evening of significant drainage. It is unclear how this might impact the cognitive findings. The patient also has retinitis pigmentosa, which seems to complicate his walking.
On 4/1/09, the patient was admitted to the neurosurgical wing of Johns Hopkins, where a Medtronic Strata valve and Aesculap Shunt Assistant (ASD) 0/20cm H20 were inserted in an occipital site. The Strata was set at 2.5 opening pressure, lowered to 2.0 on 5/1/09, and raised back to 2.5 on 7/16/09. It was lowered back to 2.0 on 7/30/09, and lowered to 1.5 on 9/10/09. During this period, there was no measurable change in ventricular size on CT, and only minimal improvement in walking and gait.
On 10/16/09, my patient was re-admitted for a second CSF drainage trial, which again produced a positive response, and it was suggested he undergo an ETV and shunt revision to lower the physical position of the (ASD) Strata valve, which was accomplished on 11/6/09. The new Strata was set at 1.5. Once at home, my patient began to experience some marked confusion, and over the following weeks, began to suffer headaches, nausea, and dizziness.
On 11/30/09, he was re-admitted to the hospital for evaluation of his dizziness by his neurologist, who found no evidence of vertigo, but mild orthostatic (postural) changes in blood pressure and slight horizontal nystagamus. He also identified some tightness and limited mobility in his neck, and suggested physical therapy to improve his range of motion. According to the records in that admission, the patient commented that the heaviness in his legs was improving, but worse in the evening. He complained of intermittent episodes of dizziness or “loopyness” throughout the day, and difficulty rising and walking from a seated position. So on 12/17/09 the Strata setting was increased to 2.0, and the next day lowered back to 1.5.
During these revisions and setting changes, it would appear there was no change in the size of his ventricles on CT, and mixed and only slight improvement in walking, balance, and gait. On 1/4/10, he met with a new neurologist at Johns Hopkins, who felt he would benefit by a lower setting, and lowered the Strata to 1.0. During this visit, the patient shared he felt overwhelmed by his health complaints, and described his NPH and cognitive changes as worrisome. He also has a history of treatment for depression.
The patient returned to the neurologist office on 1/7/10 complaining of being loopy and dizzy. His blood pressure was 162/100 and heart rate 105. His neurologist decided to leave the Strata setting at 1.0, and suggested that he seek an evaluation for a possible inner ear problem. It was not long after this that he contacted me for a consult and DiaCeph monitoring, hoping I could shed some light on a treatment plan that might better his outcome with NPH. I do not recall if he has obtained an inner ear workup as was proposed.
It would appear there has been difficulty in obtaining accurate outcomes data in my patient’s care and treatment, in part related to his blindness, staff’s inability to identify the most optimized Strata shunt setting, and apparent exacerbation of his complaints from antidepressant and amphetamine medications. In his 2/25/09 workup, the patient reported that he felt that about 25% of his gait and balance problems improved when he was off his antidepressants.
Other Relevant History:
The patient also has retinitis pigmentosa, diagnosed about 1990. He has hypertrophy of the prostate, urinary urgency, and is being treated with Flomax. He has suffered from depression for many years, and takes Tenuate Dospan. He has non-specific mild cognitive impairment, which could be dementia related, as vascular and ischemic changes are present on his brain scans. Both of his shoulders, and one of his knees, he says is in need of orthopedic surgery. Clearly, his NPH is the most significant health issue weighing on his mind.
In-Person Work-up and Observations:
This patient came to Newport Beach, California, to see me in March 2010. With a portion of his history provided in advance, I performed an initial 3 hour workup, and answered questions, discussed additional monitoring, and advised him of what could be done surgically and with shunt adjustments. We also discussed his overall health.
I performed a visual assessment of his shunt, but did not pump his valve reservoir. I took a photograph of the right side of his head of the location of his Strata valve. I performed a brief AK (applied kinesiology) finger touch exam of his shunt, using his left arm for the strength/ deficit challenge. As he has problems and weakness in both shoulders, my exam was brief, but did not reveal any pronounced elevation of ICP or deficits around the shunt that might indicate shunt failure or CSF leakage.
I discussed his maintaining an exercise regimen and how it could help his NPH and overall health. I discussed the role of a good diet, particularly, in managing caffeine and sugar intake, and moderating Tenuate so that he can sleep. I discussed the importance of maintaining regular mental, social, and physical activities and their role in long term neurological health. I described some of the modalities likely available to him under “integrative medicine.” During my workup at my home, I brought out hand drums and percussion instruments and observed him play and demonstrate good initiative in rhythmic skill, attentiveness, and creativity, at or above normal for his age. He showed me a “four-fingered beat” he plays on his hands, and I encouraged him to pursue more of these activities. I suggested that he explore what is available to him when he returns home.
I evaluated his walking and balance skill by observing him walk in his hotel room, and down a hallway unassisted, where he shuffled with feet both wide apart, and close together. I observed him walk down a hallway without shuffling, hesitation, or changes in gait when assisted arm in arm. I observed him to have difficulty with balance and initiation of steps at times and as he got up from a chair. I observed him to be “loopy” on several occasions after breakfast, and shuffling. We went for a walk and I observed him to have difficulty maintaining his balance, a sway when standing feet together in a corner, and unable to stand heel to toe.
Review of Radiographs on Disks:
I reviewed his CT and MRI brain scans. I am in agreement as seen in the x-rays that he has normal pressure hydrocephalus. I do not see much significant change, if any, in his ventriculomegaly on scan since he was shunted in April 2009. There is a slight change is in his 1/7/10 scan. He is to be rescanned again in April 2010, and perhaps this will provide more insight.
I reviewed his last lateral skull x-ray, and the Strata valve assembly can be seen with the distal portion of the valve, which houses the siphon control device, very near the “0” point, the center of the ventricles, perhaps even 1 cm plus below it. I observed the same finding in my personal exam.
Results and Discussion of DiaCeph Monitoring:
DiaCeph monitoring was undertaken with this patient from March 4, 2010 to March 15, 2010. The science behind this DiaCeph monitoring in hydrocephalus is that a patient elicits measurable non-invasive clinical “markers” which reflect shunt or ETV outcome, and severity of hydrocephalus. I review the patient’s history and complaints, identify the best markers, and create a monitoring schedule. Over a two to three week period, the marker data is collected, and then I tabulate and analyze it for ICP levels, shunt function, and shunt matching. Monitoring is usually done 5-6 times per day, for 14 to 21 days in succession. Each monitoring day produces a graph of each of the markers. Monitoring for 14-21 days assures there will be enough data points to produce an accurate distribution of the patient’s complaints. In many cases, additional event or activity monitoring is required.
A custom data “form” and user instructions were prepared for this patient. This included: 1. Walking and gait, 2. Urinary Urgency, 3.Vision, 4. Cognitive function, 5. Energy, 6. Hall Steps count, and 7. Sleep quality.
He was instructed to rate 4 of these 7 markers on a scale of normal (N), mild (1), moderate (2), and severe (3). On the Cognitive Test, he used his television to see how many TV programs out of five (5) stations he could remember after a 30 second pause. On the Hall Steps count, he was instructed to count how many steps he could briskly take in his home hallway before taking a mis-step, then to score also between N and 3. On Sleep quality, he was instructed to score as either G (good), F (fair), or P (poor), which I converted to 1-3 scoring.
Mid-way through the monitoring, my patient developed an acute problem with his left eye, leaving him without vision in that eye. He has visual impairment from retinitis pigmentosa, and the loss of vision in his left eye caused his DiaCeph data from March 9-15th to be incomplete and skewed by his distress. His data from March 4-8th appears in good order. During the 4 days he spent in Newport Beach, I was able to take a history on him, observe many of his complaints, and gain insight into his overall health.
Attached, are DiaCeph/Excel Data Graphs from March 4, 2010 to March 15, 2010, and Comparison Graphs of March 4-6 as Figures 1-4:
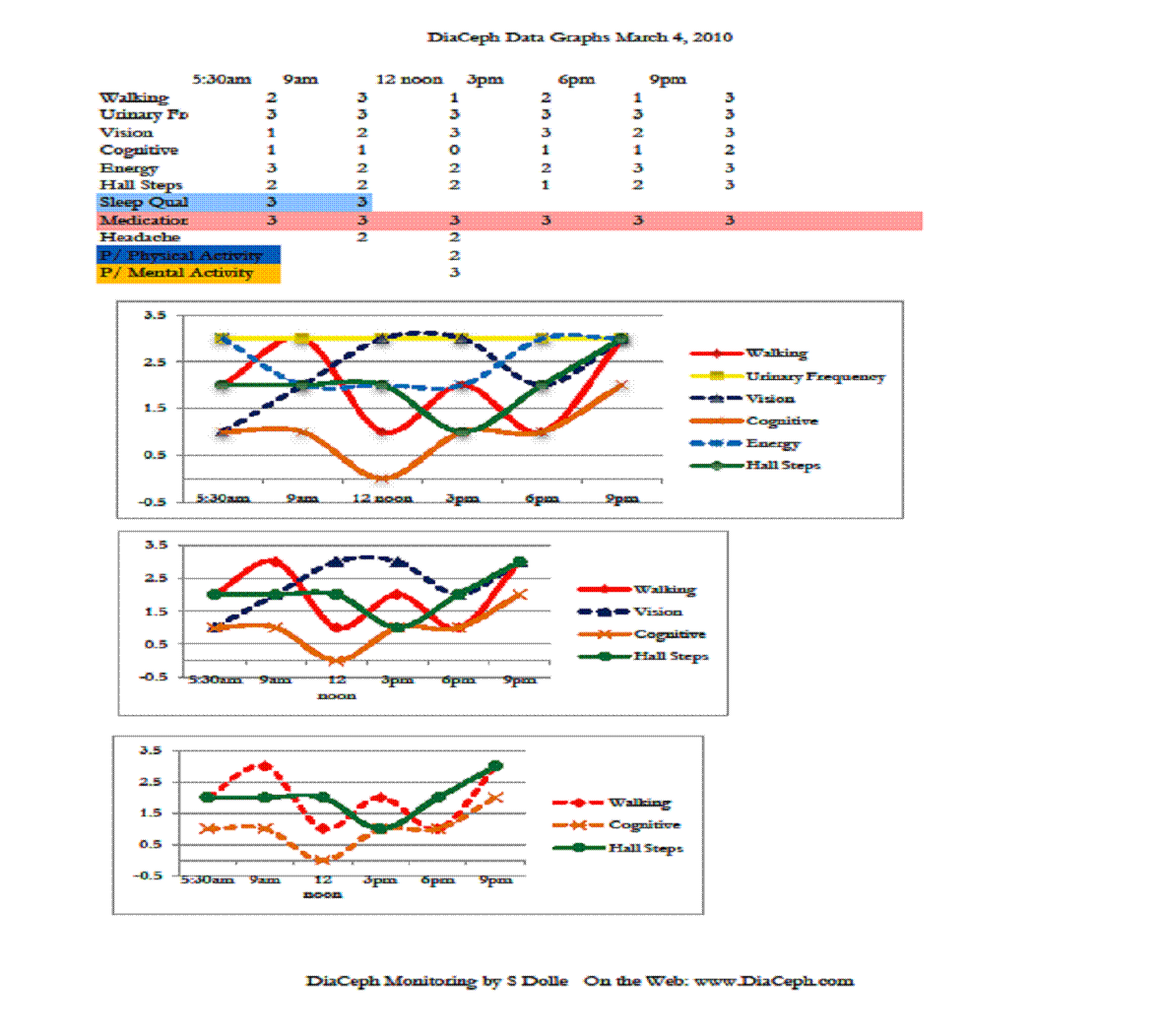
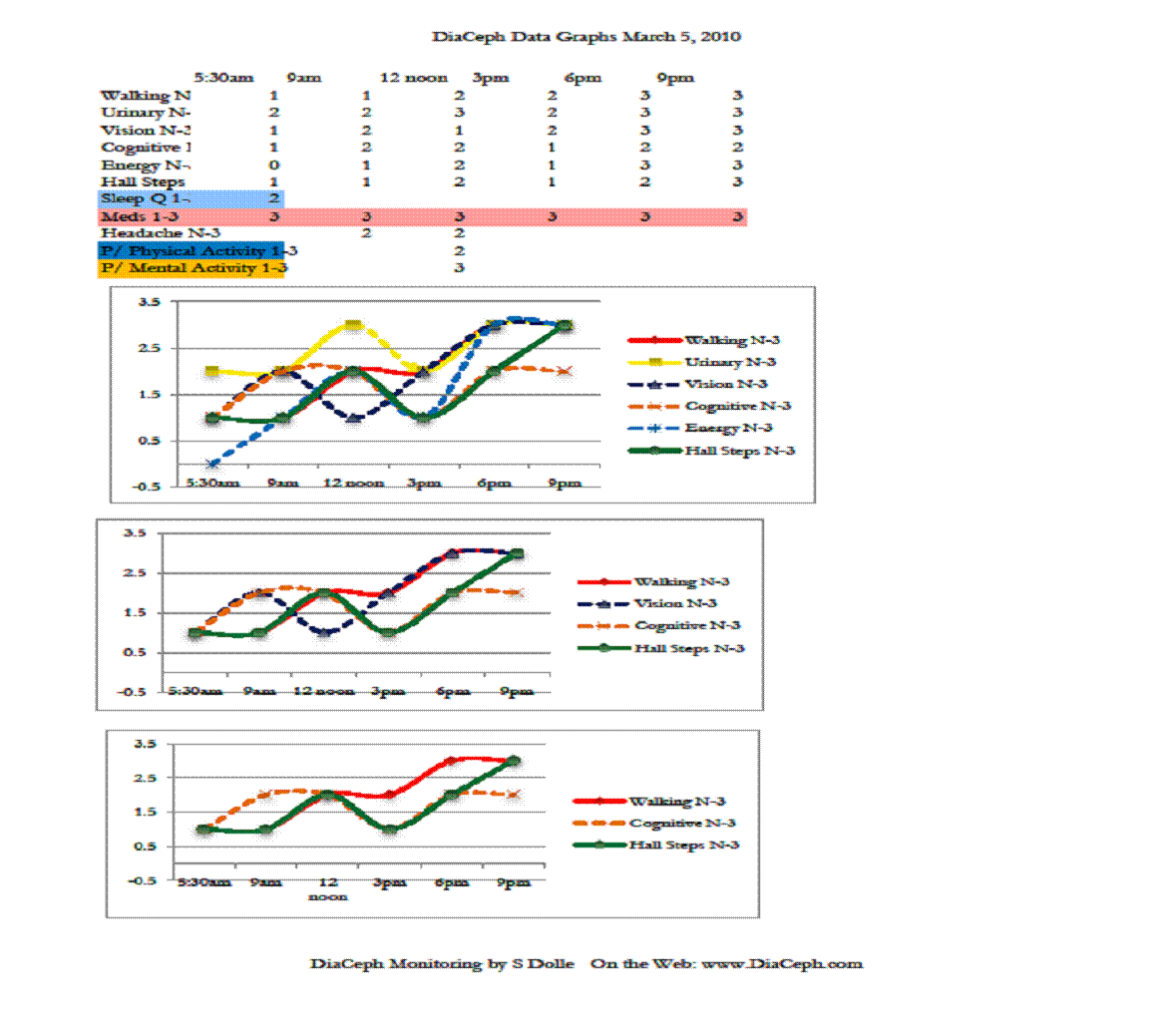
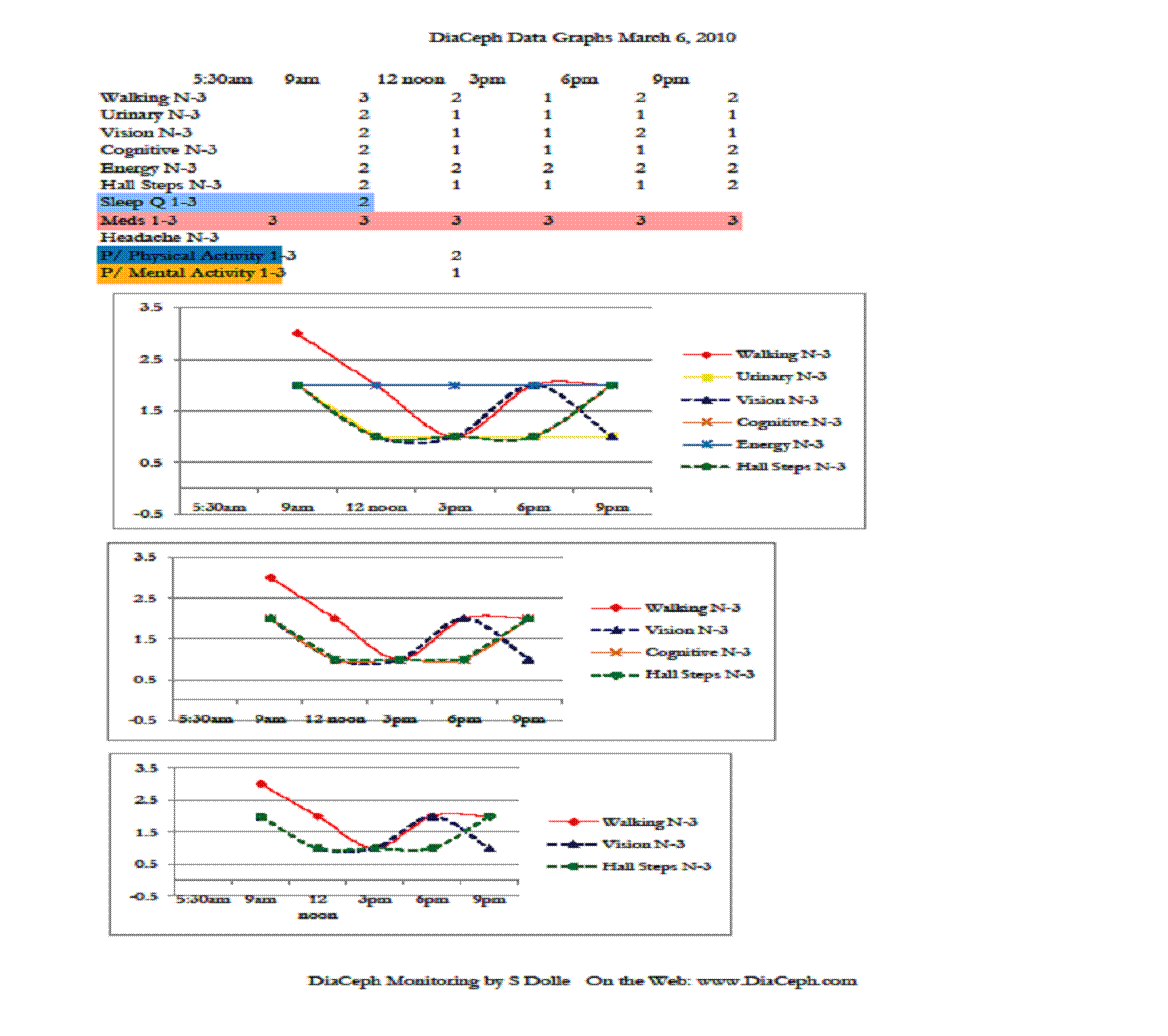
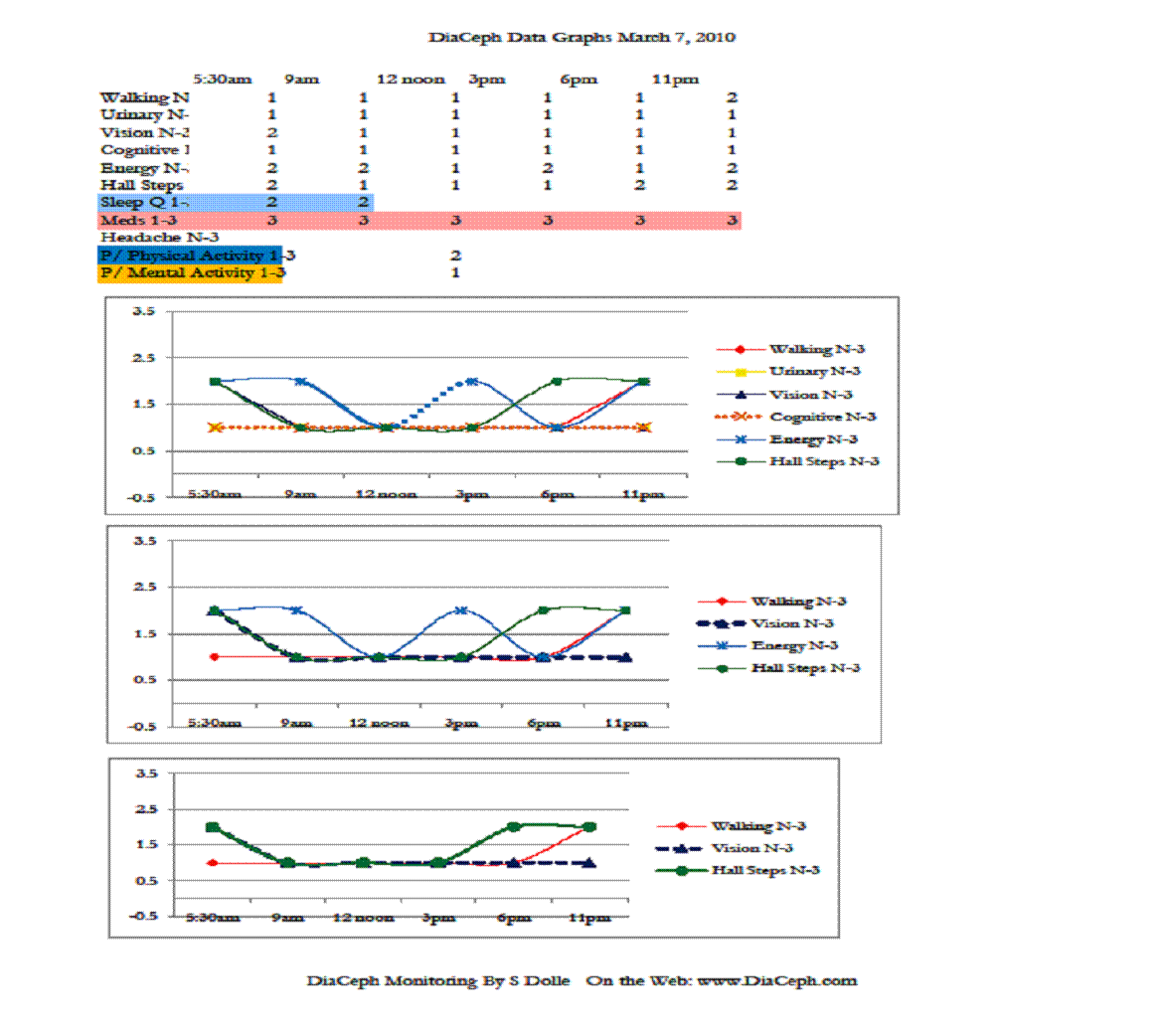
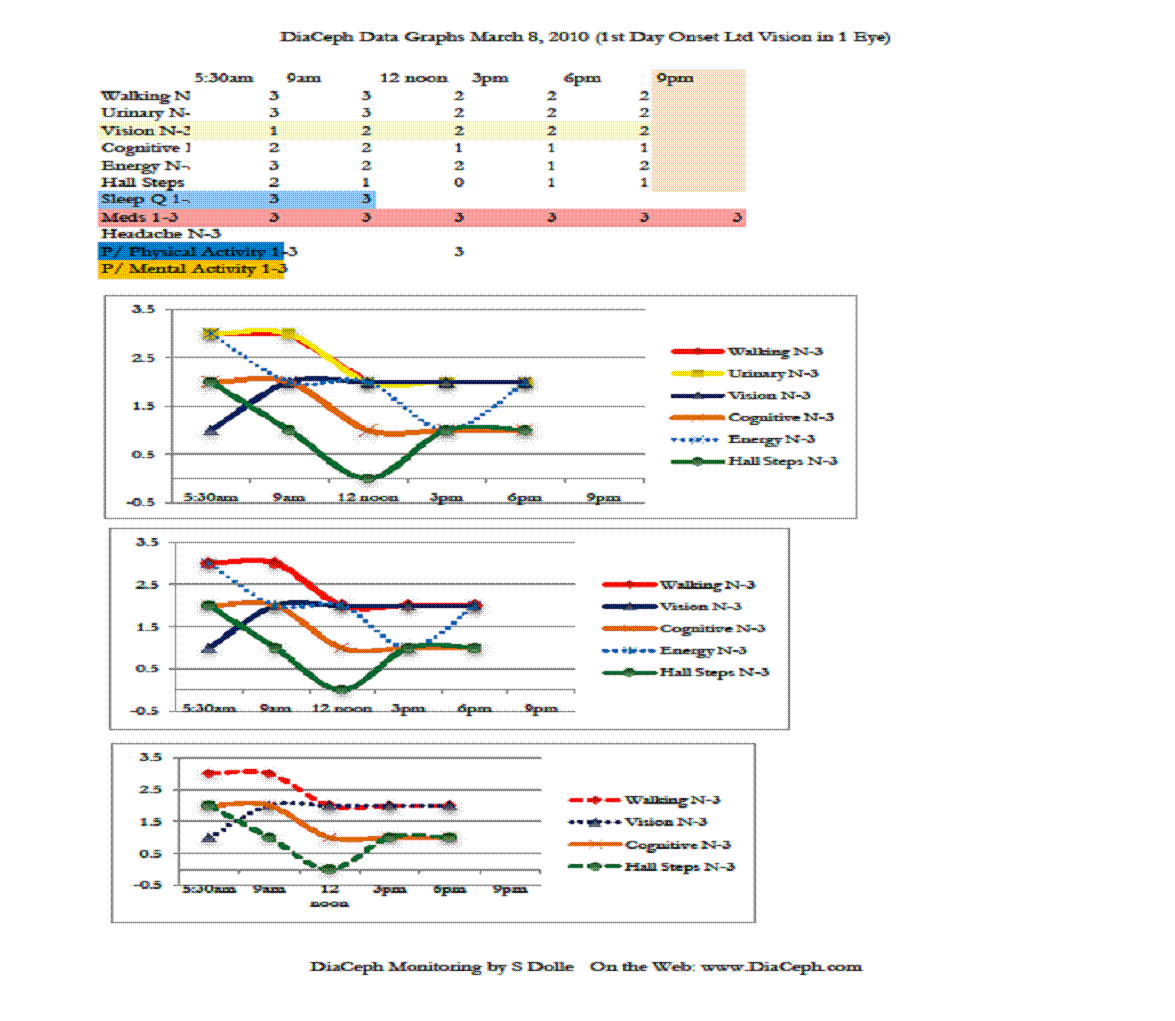
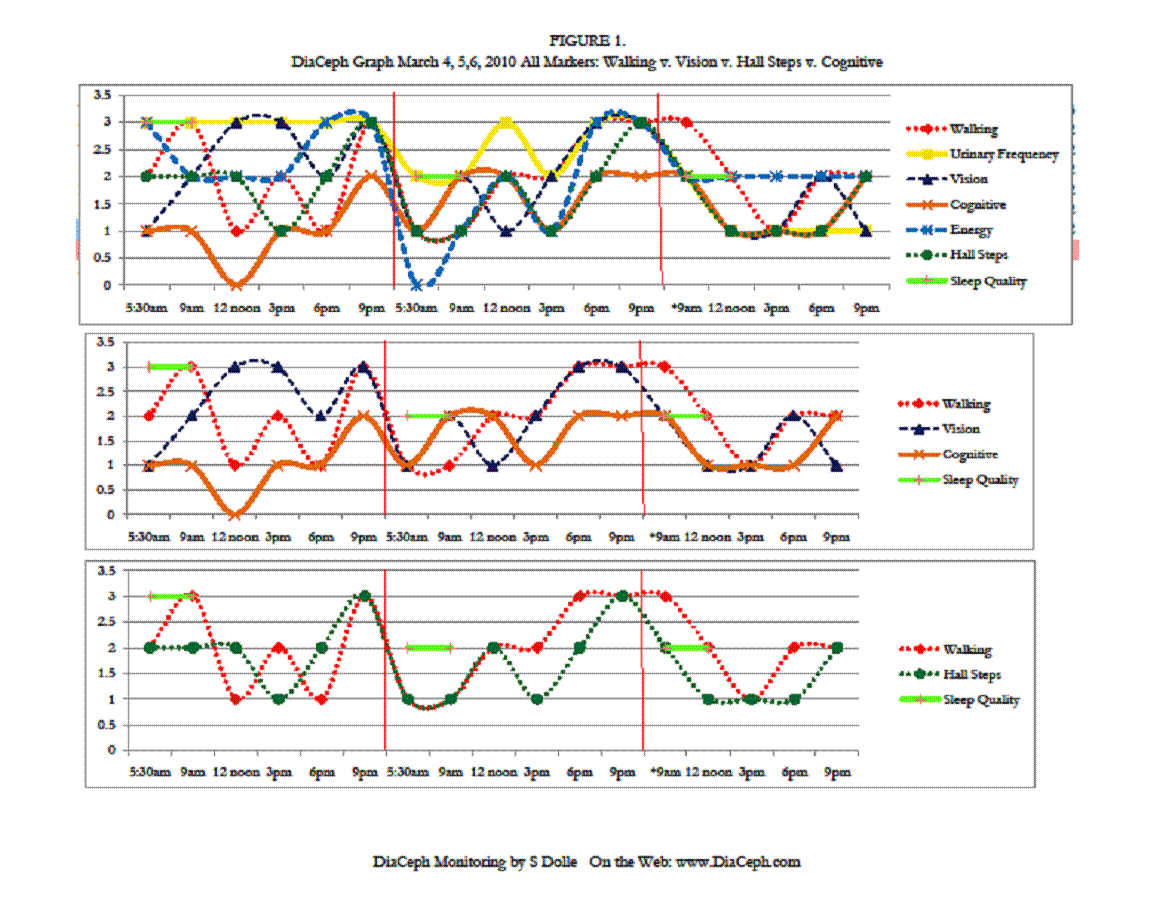
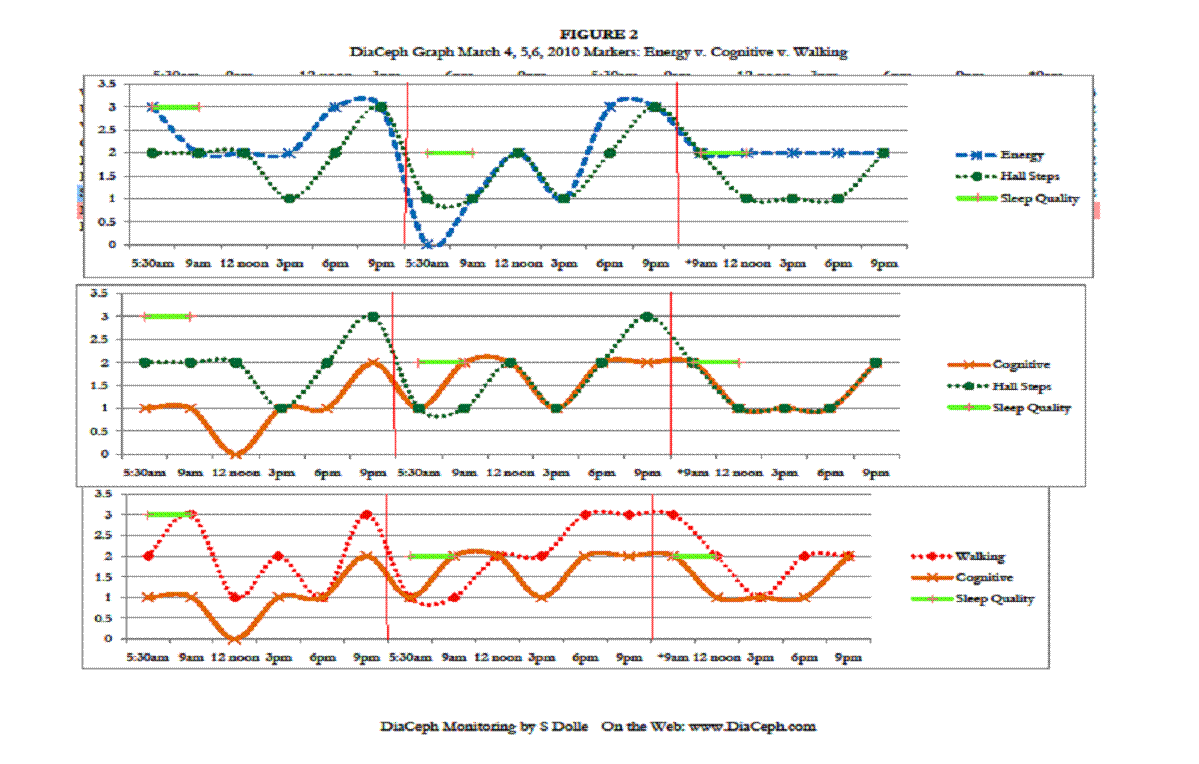
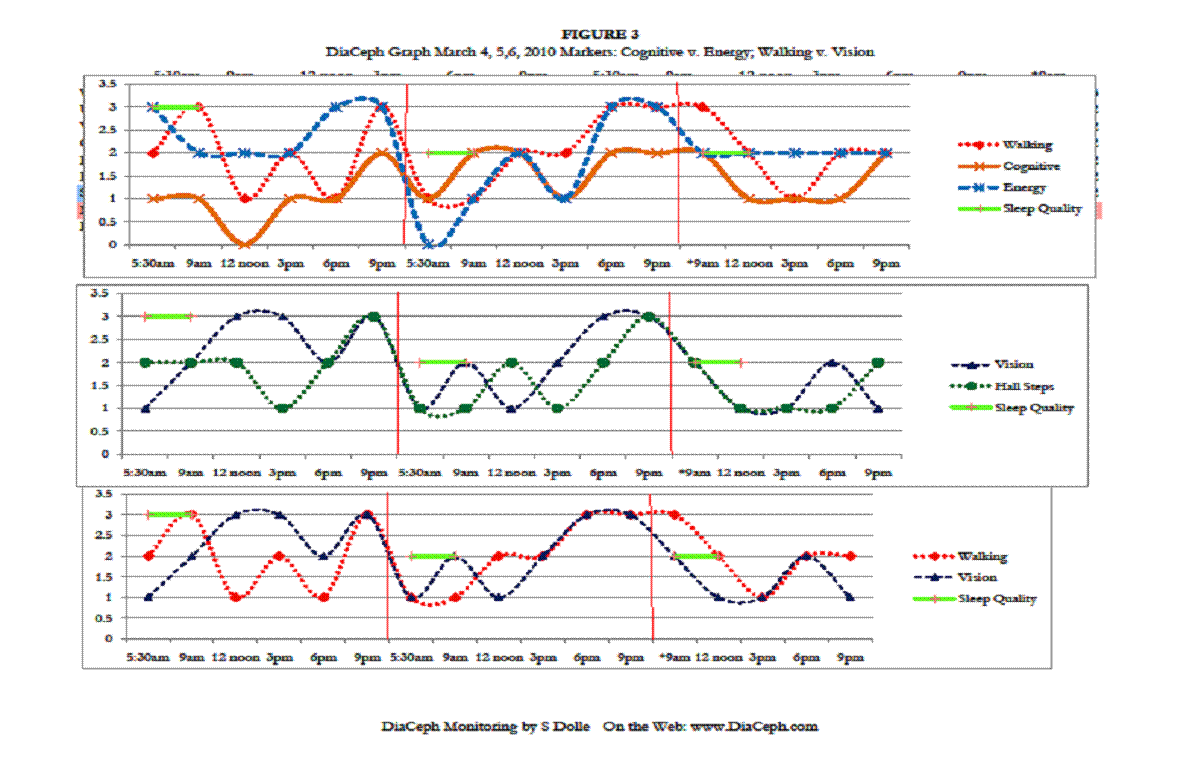

Figures 1-4 indicate his Walking curve pares closely with his Hall Steps curve, with the Walking curve slightly more sensitive to subtle changes (Figures 1. and 3.). ** Note: data points and curves higher up and away from “0” on the vertical axis (near the 3.5 line) represent abnormal findings. Points nearer to the “0” point on the vertical line represent lesser complaints, more normal findings.
Of his markers, perhaps the most telling is how well his Cognitive curve fits to his Walking and Hall Steps curves, and how they rise and worsen in the evening. The rise and fall of his Cognitive curve also mirrors his Walking and Hall Steps curves, which is consistent with NPH. However, the fluctuations in his Cognitive curves are less dramatic. This would be due to either test methodology, or that his cognitive changes are unrelated to NPH. His surgeon noted in his admission record of 11/30/09 that he was complaining of heaviness in his legs more in the evening, but that it had improved during the daytime. This would seem CSF outflow and NPH related, likely “inadequate” CSF clearance. His neurologist also noted an “orthostatic intolerance,” which may well be the loopyness he is reporting. His ongoing heaviness in his legs is likely the elevated Walking and Hall Steps DiaCeph data seen later in the day and evening. We need additional monitoring to identify his “loopyness” in the data.
The neurocognitive assessment, as part of his in-hospital CSF drainage of 3/13/09, indicated his Cognitive complaints were mild and more unrelated to NPH. My personal observation was that his cognitive difficulties seemed more like what I’ve seen in dementia. Short term memory (30 sec to 5 minutes) seems in-tact, with some difficulties with mid-term memory and recall of day to day details. Yet, this could still be related to his NPH with mild shunt mis-match per his abnormal walking scores and loopyness. I used a 5 item TV station recall Cognitive test. He informed me the test seemed too easy and that he was too comfortable with it at home, as opposed to his being put on the spot in the physician’s office. So I changed his Cognitive test to a simple observation by his wife/assistant of his memory status. I would like to see how this Cognitive finding pares with his Walking and Target scores.
My patient’s Vision curves (prior to losing sight in his left eye) do not pare as closely with the rise and fall of his Walking and Hall Steps scores. On March 4, he reported his Vision marker mid-day as rising to severe (level 3), while his Walking and Hall Steps scores were mild (level 1). On March 7, his Vision improved to mild, while his Walking and Hall Steps scores moderated between mild and moderate.
On March 15 while in Newport Beach, his Vision was so impaired he required step by step assistance in moving about his hotel room. At 5:30pm, as we headed to the hotel lobby, I observed him Walk without any shuffle, sway, or hesitation down a straight hallway arm in arm with his wife. When I asked if he could walk like this prior to his April 2009 shunt placement, both responded “no.” His Vision then was also better. I also observed him on this day to be much less bothered by Urinary urgency.
On March 15-17, I observed him having poor balance and gait episodes after breakfast and mid-day, described as “loopy” when getting up from his seat and attempting to walk. On March 16, he was unable to stand steady with feet together (in a corner) and unable to stand heel to toe. He had a pronounced shuffle as he walked with me arm in arm.
These loopy and walking complaints I suspect are due to either “fluctuations” in intracranial pressure and NPH, or elevated blood pressure and heart rate. The episodes seem to pare his abnormal Walking and Hall Steps and Energy curves. The markers are also worse later in the day and evening. It is reasonable to expect that his NPH could impact his energy. He may also have a stamina issue. His blood pressure and heart rate were reported to be 162/100 and 105 by his second neurologist on 1/7/10, yet were 138/77 and 101 on 1/4/10. His blood pressure and nystagamus findings on 11/30/09 were described as mild “orthostatic intolerance.” The patient takes a stimulant anti-depressant prescription, Tenuate Dospan. It is possible the loopy and balance episodes are blood pressure and stamina related. He also reports being loopy after exercise. I asked him if he could lower his dosage of Tenuate. On 3/25/10, I was informed it was discontinued all together, but he still continues to experience loopy episodes, notably after a long walk. In lieu of these episodes, I added a simple finger to Target circle (vestibular) test to be done 5 times a day.
His poor Sleep Quality seems to pare his Urinary urgency complaints as seen on curves in Figure 1., and pare less with his Vision, Cognitive, and Walking scores (Figures 1, 2, 3, and 4).
In a limited number of days of monitoring, the patient’s DiaCeph results seem to indicate an intermittent exacerbation of his gait and walking complaints, likely due to NPH and suboptimal CSF clearance and shunt performance, but elevated blood pressure and heart rate as a cause, cannot yet be ruled out. It is difficult to state with any degree of certainty (with the limited number of days), whether his suboptimal outcome is due to overdrainage, or underdrainage. His history would indicate the latter. He has a double-ASD shunt system that could lend itself to upright underdrainage. As his Strata valve was gradually lowered, he did experience improvement in gait and walking complaints. It is presently set at 1.0. A trial period of 3-10 days at the 0.5 is a possibility. I would suggest additional monitoring to best understand his complaints, and avoid further complication and guesswork.
This monitoring should include:
1. Seven (7) more days of monitoring using the 4th Version DiaCeph Form, with Blood Pressure, HR, and Target circle monitoring.
2. Activity monitoring of loopy episodes, after exercise, and after spending a portion of the day in a supine posture (i.e. on the couch).
Impression:
1. Improving but unresolved walking and gait complaints, confirmed by treating physicians, by my own observations, and in a limited number of days of DiaCeph monitoring. This would appear to be due to NPH, inappropriate CSF clearance, and sub-optimal shunting to date. His reported heaviness in his legs later in the day and evening seems to fit his abnormal Walking, Hall Steps, and Cognitive DiaCeph scores, consistent with NPH and undershunting. Lowering of his Strata setting and/or revision of his double ASD shunt system might be indicated.
2. Orthostatic changes presenting as dizziness and loopyness, likely due to age, blindness and physical inactivity, anxiety, shunt drainage and the number of reoperations/shunt adjustments in a relatively short period of time. This is likely the pattern seen in improving gait scores, not as much in TUG scores. It would appear his anxiety is fueled by his complaints not having been resolved to date, and is likely his reason for contacting me in California. I believe integrative medicine therapies and exercise would likely help these complaints.
3. Lowering of his Strata valve at this juncture seems indicated, but should be weighed against his ongoing anxiety and orthostatic challenges. Further DiaCeph monitoring would help minimize guesswork and exacerbation of his status.
4. Possible exacerbation of orthostatic complaints from the use of antidepressant medication and amphetamines, and Flomax.
5. Mild cognitive changes per neuropsych exam and in-person assessment possibly due to NPH, though more likely related to dementia in view of the vascular changes seen on CT and MRI brain scans. His 3/13/09 in-hospital CSF drainage trial presents some confusion as to when his baseline cognitive score was obtained during drainage, and how this might impact his cognitive and dementia diagnoses. Limited days of DiaCeph monitoring confirmed that his cognitive changes do pare with his walking complaints, more consistent with NPH. It is unclear at this juncture how much of his cognitive complaints might abate if he were optimally shunted.
6. Neuromuscular changes and limited mobility in his neck, likely due to age and sports and injury history, which I did not work up, but would seem to be adding to his physical inactivity, and fueling his post shunting orthostatic challenges.
7. My patient is a wonderfully intelligent, cooperative, and talented 70 year old man, who should respond well to most treatments and therapies. As with any surgical or therapeutic intervention, care should be taken so as to not overwhelm the patient with the intervention(s). I believe this is what occurred with his bout of confusion following his 11/6/09 ETV and shunt revision. Given his eagerness to cooperate, and his present orthostatic challenges, I believe integrative therapies like acupressure, Tai Chi, and meditation/ visualization may help him, as well as physical exercise and social activity.
Recommendations:
1. Continue with DiaCeph monitoring as described.
2. Continue treatment for his failed eye lens and retinitis pigmentosa.
3. New integrative medicine therapies and exercise for orthostatic complaints.
4. New management and moderation of antidepressant, amphetamine, and Flomax medications. I am informed he has discontinued the Tenuate medication.
5. Increased integration in social activities and personal interests.
6. Physical therapy and home exercises to improve mobility in his neck, and help address acute complaints in his shoulders and knee.
7. Discontinue fluids two hours before bedtime.
8. Lower his Strata setting to 0.5 if/when indicated by additional monitoring.
9. Meet with a nutritionist to help moderate dietary intake of animal fats (prostate health), sugars, and caffeine.
10. Daily vitamins, including, saw palmetto.
11. Re-evaluation of his cognitive complaints at the appropriate time.
12. If further adjustment of his Strata valve and exercise/integrative medicine therapy does not provide relief, I suggest a revision of his double ASD shunt system to a Codman Hakim valve with or w/o Shunt Assistant, a Strata NSC with or w/o Shunt Assistant, or a Diamond Valve.
Attached, please find his DiaCeph/Excel Data Graphs from March 4, 2010 to March 15, 2010, and Comparison Graphs of March 4-6 as Figures 1-4.
Per instructions from my patient, a copy of this report and a summary letter were mailed to his 3 Johns Hopkins treating physicians.
I will append this report with a letter when new DiaCeph data is made available.
By:
____________________________
Stephen M. Dolle
Inventor, DiaCeph Test for Hydrocephalus
Neuroscientist, Medical Consultant & Patient Advocate